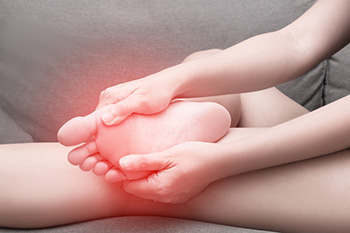
Wearing shoes that do not fit properly is a leading cause of foot pain as well as long-term complications. Tight or loose footwear can lead to corns, calluses, and even foot deformities, such as bunions or hammertoes. Over time, discomfort may limit mobility and discourage regular activity. Ill-fitting shoes can also worsen conditions like peripheral neuropathy by adding pressure and irritation to sensitive areas. A podiatrist can examine your foot shape, assess any damage, and recommend properly fitting shoes or custom orthotics to relieve pain and prevent further issues. If you have developed foot pain from wearing the wrong type of shoes, it is suggested that you schedule a visit with a podiatrist who can treat various foot conditions and offer the right guidance for your specific needs.
Foot Pain
Foot pain can be extremely painful and debilitating. If you have a foot pain, consult with Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Causes
Foot pain is a very broad condition that could be caused by one or more ailments. The most common include:
- Bunions
- Hammertoes
- Plantar Fasciitis
- Bone Spurs
- Corns
- Tarsal Tunnel Syndrome
- Ingrown Toenails
- Arthritis (such as Gout, Rheumatoid, and Osteoarthritis)
- Flat Feet
- Injury (from stress fractures, broken toe, foot, ankle, Achilles tendon ruptures, and sprains)
- And more
Diagnosis
To figure out the cause of foot pain, podiatrists utilize several different methods. This can range from simple visual inspections and sensation tests to X-rays and MRI scans. Prior medical history, family medical history, and any recent physical traumatic events will all be taken into consideration for a proper diagnosis.
Treatment
Treatment depends upon the cause of the foot pain. Whether it is resting, staying off the foot, or having surgery; podiatrists have a number of treatment options available for foot pain.
If you have any questions, please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
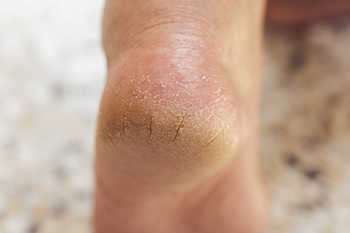
Cracked heels occur when the skin on the bottom of the feet becomes excessively dry and thick, leading to painful splits or fissures. Dry skin can be caused by prolonged standing, wearing open-back footwear, cold weather, or lack of moisture. Over time, the dryness may worsen and the skin loses elasticity, eventually leading to deep cracks that can cause discomfort, bleeding, or infection. Symptoms include rough patches, flaking, redness, and pain while walking. A podiatrist can assess the severity, remove thickened skin safely, recommend moisturizing treatments, and address any complications. If you are experiencing discomfort from having cracked heels, it is suggested that you schedule a visit with a podiatrist to restore smooth, healthy skin, and prevent further damage.
If the skin on your feet starts to crack, you may want to see a podiatrist to find treatment. If you have any concerns, contact Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Cracked Heels
It is important to moisturize your cracked heels in order to prevent pain, bleeding, and infection. The reason cracked heels form is because the skin on the foot is too dry to support the immense pressure placed on them. When the foot expands, the dry skin on the foot begins to split.
Ways to Help Heal Them
- Invest in a good foot cream
- Try Using Petroleum Jelly
- Ease up on Soaps
- Drink Plenty of Water
Ways to Prevent Cracked Heels
- Moisturize After Showering
- Skip a Shower
- Keep Shower Water Lukewarm
- Don’t Scrub Your Feet
If you are unsure how to proceed in treating cracked heels, seek guidance from a podiatrist. Your doctor will help you with any questions or information you may need.
If you have any questions, please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot care needs.
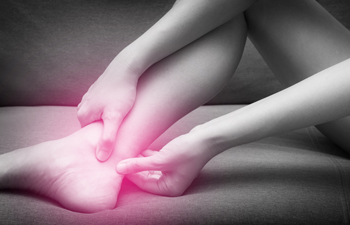
Achilles tendon injuries involve damage to the strong band of tissue that connects the calf muscles to the heel bone. These injuries are often caused by overuse, sudden increases in activity, or tight calf muscles. Risk factors include poor footwear, flat feet, and inadequate stretching. Symptoms may include pain, swelling, stiffness, or a feeling of weakness in the back of the ankle. Types of Achilles injuries include inflammation of the tissue surrounding the tendon and degeneration of the tendon itself. A podiatrist can provide targeted treatment through custom-made orthotics and preventive education. If you experience persistent Achilles pain, it is suggested that you consult a podiatrist who can accurately diagnose and treat this condition.
Achilles tendon injuries need immediate attention to avoid future complications. If you have any concerns, contact Thomas Vail, DPM of Step Alive Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Is the Achilles Tendon?
The Achilles tendon is a tendon that connects the lower leg muscles and calf to the heel of the foot. It is the strongest tendon in the human body and is essential for making movement possible. Because this tendon is such an integral part of the body, any injuries to it can create immense difficulties and should immediately be presented to a doctor.
What Are the Symptoms of an Achilles Tendon Injury?
There are various types of injuries that can affect the Achilles tendon. The two most common injuries are Achilles tendinitis and ruptures of the tendon.
Achilles Tendinitis Symptoms
- Inflammation
- Dull to severe pain
- Increased blood flow to the tendon
- Thickening of the tendon
Rupture Symptoms
- Extreme pain and swelling in the foot
- Total immobility
Treatment and Prevention
Achilles tendon injuries are diagnosed by a thorough physical evaluation, which can include an MRI. Treatment involves rest, physical therapy, and in some cases, surgery. However, various preventative measures can be taken to avoid these injuries, such as:
- Thorough stretching of the tendon before and after exercise
- Strengthening exercises like calf raises, squats, leg curls, leg extensions, leg raises, lunges, and leg presses
If you have any questions please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.

Foot and ankle fractures are fairly common in children, especially those who are active in sports or play. These injuries happen when one or more bones break due to a fall, twist, or direct hit. Signs may include swelling, bruising, trouble walking, or the child refusing to put weight on the foot. Because children’s bones are still growing, some fractures affect growth plates, which are areas near the ends of bones that help shape future bone development. Treatment depends on the location and severity of the break. Some injuries may heal with rest, a cast, or a boot, while others may need more involved care to make sure the bones heal in the correct position. If your child has foot or ankle pain after an injury, it is suggested that you see a podiatrist to make sure proper healing can begin.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Thomas Vail, DPM from Step Alive Foot & Ankle Center. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
- Bruising
- Pain
- Redness
- Swelling
- Blue in color
- Numbness
- Cold
- Misshapen
- Cuts
- Deformities
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our office located in Findlay, OH . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
